Ask The Placenta Lady is a show about the birth year. Pregnancy, birth, and postpartum recovery – no question is too strange for The Placenta Lady!
Our question for this episode is: “How can I have a successful VBAC?”
Joining us today is Aundrea Moore, PBi Placenta Encapsulation Specialist®. Aundrea had a VBAC with her second child, and shares what she did to make it a success. She also shares what happened during her first pregnancy and birth that ultimately led to a Cesarean delivery.
Listen to the podcast:
Full Transcript:
Hi, welcome to another episode of Ask the Placenta Lady. My name is Jodi, but I’m usually just called The Placenta Lady. I’ve been working in the field of postpartum support since 2006, and I’ve heard pretty much everything under the sun, which is why our tagline is “no question is too strange for the Placenta lady.”
Joining me today is Aundrea Moore. Aundrea is a PBi Placenta Encapsulation Specialist® in upstate South Carolina. Welcome to the show, Aundrea. Why don’t you tell us a little bit about your business?
[Aundrea]: Thanks for having me, Jodi. It’s so great to be here. Yes, I am in upstate South Carolina. I became a PBi Placenta Encapsulation Specialist® about a year ago. And I’m in the Greenville area, although I travel around. And I love to be a part of the birth community, especially PBi.
[Jodi]: That’s awesome, Aundrea. And thanks for being here today. Our question for this episode is, “How can I have a successful VBAC?”. For those that don’t know, it stands for Vaginal Birth After Cesarean. So this is a great option for women.
I know that in the past, the phrase has been “once a Cesarean, always a Cesarean”. And that is not necessarily true. So it’s important to know your options, to ask about them and see what is possible for you.
So Aundrea, you had a VBAC with your second child?
[Aundrea]: Yes, I did, correct, with my second child. My first child was a planned unmedicated vaginal birth. However, I did not educate myself and how I needed to plan for that. I wasn’t aware of my, I wasn’t informed of the decisions and the options that I had. So after I had my C-section, my doctor the first time around actually told me, “you’ll never be able to have a vaginal birth again”.
At first I just believed it. I’m like, okay, I’ll just have another C-section. I’ve been through it once. I know what to expect. But once we got pregnant again, I just really began questioning, like, I don’t think that’s true.
Tips for a Successful VBAC

So the very first thing that I did when I became pregnant was I found a VBAC-friendly, supportive provider, which was a local midwifery group here. I had a first appointment with them and told them, this is what I’ve been told. This is what I’ve been through. Their reasoning for me not being able to have another vaginal birth was my bone structure. It wasn’t going to allow him to come down. And my first baby got stuck the first time, is what they told me.
So I was asking the midwives, I said, “Is this true? Am I going to be able to have a vaginal birth, or do I truly have a bone structure that’s not going to allow it?” And she just kinda laughed. She was like, “Of course! You’re a great candidate. Everything checks out.” So that was the very first thing I did, was I found a provider that was supportive of a VBAC and my desire to have one.
From there, I hired a doula, who just so happens to be another PBi Placenta Encapsulation Specialist. She encapsulated for my first and my second child. So she was becoming a doula, so I hired her. And she was absolutely wonderful. She met with us throughout my pregnancy, helped my husband, really I think the biggest thing was she guided my husband in how he could be of help.
The first time, my husband had no idea, he had no clue what to do or how to help me, especially because I was confined to a hospital bed, hooked up to all these wires. The plan was for me to labor at home as long as possible. So she came over and kind of guided us through different positions that we could try during labor. And he felt very included. He wasn’t just a bystander. He was a participant in our labor and birth. And that made him feel really good. Those were the first two things I did.

Because of my so-called bone structure issue, I decided to go to a chiropractor. Admittedly, I had never been to one in my life, no one in my family had gone. So I decided to seek out a chiropractor, and a Webster-certified one. I began seeing her in my second trimester, and I saw her from there on out. She did tell me that one side of my sacrum was constantly off, so every time she did adjust. I did that all the way up until I think two days before I gave birth to him.

I educated myself. I read a lot of positive VBAC stories. I surrounded myself with people who were supportive and ignored those who weren’t. I read a lot from the ICAN website, the network.

I listened to some Hypnobabies things as well, to give me a positive mindset. Admittedly, I struggle with my mentality sometimes. So I wanted to constantly hear the positivity whenever I began to doubt myself. So I listened to some Hypnobabies tracks. I never was able to actually take the classes. I did my own birth affirmations on postcards. It was very relaxing to sit there and do it and to constantly read through them and see them daily and know that that was going to be ingrained in my head.

And then I did a lot of Spinning Babies movements to try to get him in the most optimal position I could. He did, up until toward the end, like to flip. He was breech at one point. He flipped transverse. He really kept things interesting, also known as stressing me out. So I did a lot of Spinning Babies movements and walking.
And then I think the last thing that we had planned was to labor at home as long as possible. Here in South Carolina, if you’re a VBAC, you’re required to give birth in a hospital. Birth centers and home births are not an option, which is unfortunate. I hope that that changes in the near future. So even though I would have the support of a doula, and knowing that my midwives were there for me, I also just know that a hospital setting in general, there are also nurses there and other people who might push things on you. Especially if you’re in transition or something, and they so much as mention epidural, that sounds really appealing, even if you don’t want that. So I labored at home until I hit transition.
In fact, my doula had to force us to leave, because I was like, “Nope, I’m not going anywhere. I don’t wanna sit in a car, (’cause the hospital was about 30 minutes from my house.) And so I was like, I’m not sitting in a car for 30 minutes. You guys are crazy.” So she, finally, after one contraction, I remember in the video that my photographer took, my doula looked up at my husband and said, “We gotta go!”, because she knew we were getting close. It’s funny that that’s videotaped. But so we did, we got to the hospital when I was seven centimeters dilated. And he was born about an hour after we got there.
The birth itself wasn’t exactly as planned, not because of anything forced on me. It was just that unfortunately he did have a nuchal cord, which is very, very common and most of the time is not an issue at all. For him, it was. It was compressing his neck, and his heart rate was dangerously low. It got kinda scary for a while.
But the whole time I felt very supported. Even though I wasn’t gonna be able to get in the water and have the water birth that I so much desired, the midwives were wonderful. My doula and my husband were wonderful. He did arrive safely. He spent a day in the NICU. But all was well.

It was the most empowering experience of my life, to just know that I trusted my body, even when I doubted it a couple of days prior, you know? Here, and most places, if you’re a VBAC, you can only go two weeks overdue. And so he was 12 days overdue. So we were two days away from that cutoff. And I had a breakdown about two days prior to his birth. I was just like, maybe my body really can’t do this. He still feels high. I’m scared.

And that was when my doula, I will say again, was just amazing, because she checked on me that day, and I was honest with her. And she was just so supportive. I can’t say enough how important I feel a doula is for anyone, whether it’s a C-section or a planned epidural birth or an unmedicated. They’re amazing. They really are. So we did, we had an unmedicated VBAC.
And I remember after he was born, the midwife who caught him said, “I don’t know what your previous doctor was talking about. You have an amazing pelvis to give birth.” And it was really just such a nice thing to hear, that not only did I do it, but my body is capable of this. It’s made for this. And then in the future, if we choose to have more children, there’s that option again. And so it was a wonderful experience.
It was such a nice thing to hear, that not only did I do it, but my body is capable of this. It’s made for this.
[Jodi]: That is really awesome, Aundrea. I really appreciate you sharing that story and your experience. I just wanted to add just a couple things. You mentioned ICAN, and ICAN is an amazing resource. It stands for International Cesarean Awareness Network. And for those watching, you will have an ICAN chapter in your city and state. So if you’ve had a Cesarean birth and would like to talk to other women who have a similar story and kinda process that, a lot of different emotions come up around that. And sometimes you just need to talk to somebody about your experience and just get that kind of camaraderie and support, and even validation.
The other thing I was just going to throw in, for those that don’t know, a nuchal cord is where baby presents with the umbilical cord wrapped around the neck. And it is very common. And a lot of times it just rectifies itself.

The other thing that I really appreciated you mentioning was, yes, the doula, and also the positive birth affirmations -somebody just telling you that your body works, and you can do this. It makes an incredible difference for birthing people to just hear that you can do this, and you’re not broken. And if you’re around or surrounded by people who are unsupportive of your desires to attempt a VBAC, then I would definitely seek out a birth doula.
Hypnobabies and Hypnobirthing is another wonderful option. It’s a lot about that validation, the mental process and feeling that you can do this and you will do this. And birth, like so many other things, yes, it’s physical. But it’s also extremely mental. You have to kinda get out of your own way as far as believing in yourself. It’s one of the hardest things that we can do physically. I mean, I know people run marathons and things like that. But you do hit a wall. And just hearing, “You can do this and you’re not broken” is so essential.
It should be common in hospital births that women are encouraged, and told that they CAN birth their baby. It makes a huge impact.
I wish that was just common in birth settings and particularly hospitals, that women are encouraged. Instead of having these negative stories being told to women, especially when they’re in the throes of trying to do the hardest thing they’ve ever done. It just makes a huge impact. So I really appreciate you bringing that up, as well, because it is so essential.
So I understand you had a Cesarean delivery with your first child. You know they say hindsight is 20/20… Do you want to explain a little bit about what your provider was saying, and the events that led up to you having that style of birth?
Avoiding a Cesarean Birth: Know the Signs
[Aundrea]: So with my first, I hadn’t spoken with many women who had given birth. So I didn’t realize that once I was approaching my due date how much they would start pushing and mentioning induction. So I went to my 39 week appointment, and she was like, all right, when you come in for your 40 week appointment, we’ll start seeing where you are and start talking about induction. So I went in for my 40 week appointment, and she said, “If you haven’t made any progress, we’ll go ahead and schedule your induction for the end of the week.”, which would have been around 41 weeks.

I didn’t know that I had a choice. I think that’s one thing I definitely wish more women knew, is that you don’t have to show up for an induction if it’s not medically, if there’s not something harming you or your baby. If the doctor’s pushing it on you, you can say, no, let’s wait a little bit longer, as long as all is well.
I didn’t know that I had a choice [to refuse induction].
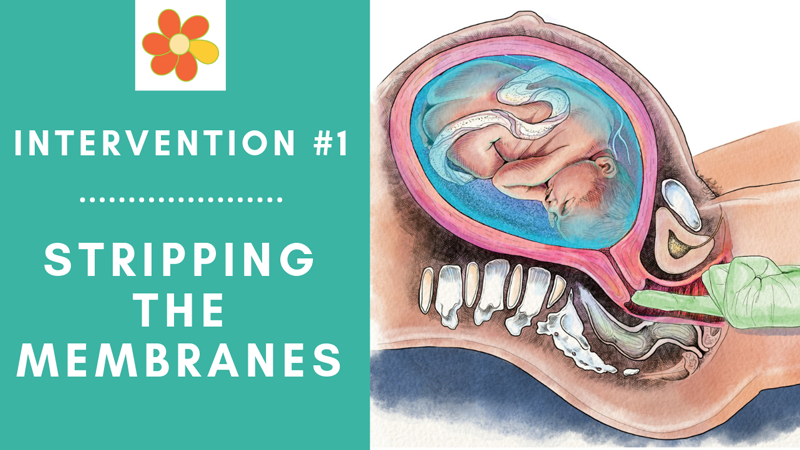
So the other thing, I had no clue what stripping your membranes meant. And so I went in at 40 plus something, and she was checking to see my dilation, which hadn’t progressed really at all, and she said, “Let’s just go ahead and strip your membranes and see if we can get things going.” And I was like, okay. I mean, I was definitely ready to have my baby. I just didn’t realize that waiting for my body to be ready and my baby to be ready would be so important in the labor and delivery process.
So she stripped my membranes, and it was later that day that I started having sporadic contractions. And then early the next morning, my water actually broke. However, I truly believe my body just wasn’t ready. But the stripping of the membranes agitated things enough to try to get it going, because once I got into the hospital, they only admitted me because my water had broken.
Once I got there, my labor stalled completely. In fact, she asked me what my birth plan was. And I said an unmedicated birth. And she said, “Oh, that’s generally best the second time around. So let me know when you’re ready for your epidural.” So right from the bat, my body just seized up. I’m not supported in what I had envisioned in my head already. And so that’s actually when my labor stalled.
So then the Pitocin got started. And then once the Pitocin got started and I was laboring on that for three or four hours and hadn’t progressed much, I was already exhausted ’cause it had been about 24 hours since everything had kinda gotten started, and went ahead and gave in to the epidural.
And then of course with the epidural there are also some things, it can be of great benefit to those who want it or need it. But there are also downsides, and I had some of the downsides. And so did my baby. His heart rate was not doing well. So I did fully progress, and I did get to push. But that’s when he got stuck, and they said that my bone structure just wasn’t supportive of a vaginal birth.
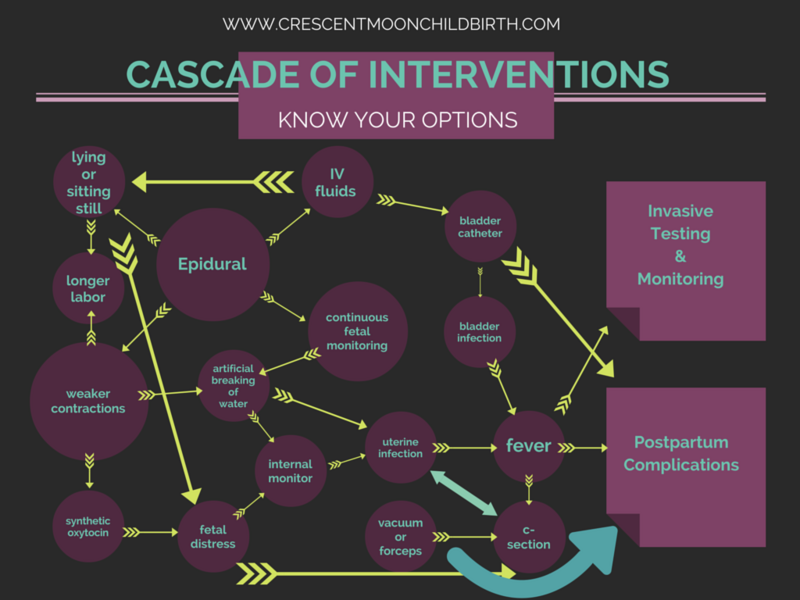
[Jodi]: Unfortunately, your story is quite common, as far as these things that can lead up to a Cesarean delivery. What they tend to call this is a cascade of interventions. And once that starts, one intervention leads to the next one, leads to the next one, until surgical delivery.
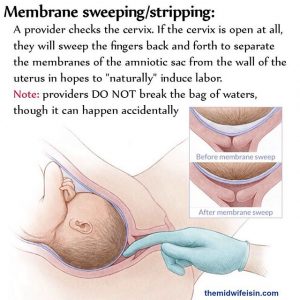
Stripping of the membranes is where your care provider, and midwives do it too, is gloving up and swiping / sweeping their finger between the membranes of the amniotic sac that your baby is housed in and your uterus. So they reach in there, and they do this little swiping motion, and they call it stripping the membranes. And it can lead to induction of labor. And so that’s usually the first intervention.
So I think what is a good takeaway, if you’re currently pregnant and seeing a care provider, and typically an OB, but again, some midwives are happy to do interventions as well, is just to kind of hear (pay attention to) these things. They start mentioning induction at 38, sometimes even 36 weeks, which obviously is not based on evidence.
We talk a lot about evidence-based care. And unfortunately a lot of what happens in our standard practice of care, particularly in hospitals with OBs, is they do things that are either they’ve always done, “we’ve always done it this way”, or it’s hospital policy to do it this way. And it really isn’t based on the actual research that has been done into that practice. As far as constant fetal monitoring, [induction, multiple interventions]… all of these things don’t necessarily lead to better outcomes for mothers and babies. And that is really unfortunate.
And once you start with one intervention, as Aundrea’s story and so many other stories of Cesarean delivery start, is that it starts with that stripping of the membranes. It starts with talk of induction, because then they just kinda keep setting you up so that when it does become, “Well, we need to do a Cesarean in order to save your baby”, then you’re already prepped to accept that story.
Obstetricians are surgeons. And if you go to a surgeon to have your baby… well, they like to perform surgery.
Obviously, Cesarean is a wonderful method for getting the baby out in an emergency situation. But the World Health Organization says that about 10%* of deliveries would require a Cesarean birth. However, some hospitals have 50% Cesarean rates. And that’s obviously not based on actual need or necessity. Obstetricians are surgeons. And if you go to a surgeon to have your baby, they like to perform surgery.
The World Health Organization says that about 10%* of deliveries would require a Cesarean birth. However, some hospitals have 50% Cesarean rates. And that’s obviously not based on actual need or necessity.
So again, thank you for sharing your story with us, Aundrea. If somebody wants to reach out to you, either to talk about VBAC or Cesarean birth or your services as far as placenta encapsulation or anything else, where is the best place for people to get a hold of you?
[Aundrea]: My business pages are both on Facebook and Instagram at MooreBirthServices. Birth serviceS because in the future I do want to add becoming a birth doula and maybe some other options to it, as well. But currently placenta encapsulation is absolutely my passion, and I love it. I did have my placenta encapsulated with both of my children, as I mentioned. And I would do it again with a third in a heartbeat. So those are the two places that I can be reached.
[Jodi]: That’s awesome, Aundrea. And I would just like to thank you for watching this episode of Ask the Placenta Lady. If you are looking for a PBi Placenta Encapsulation Specialist in your area, an easy URL for that is just Placenta.Directory. You can find somebody in your area to prepare the placenta for you.
Thank you for joining us, and remember, no question is too strange for the Placenta Lady! And you can ask your questions at AskthePlacentaLady.com.
We’re also on Facebook at Placenta Benefits. I’m on Twitter @PlacentaLady. And Instagram @PlacentaBenefits. Thank you so much.
——————————–
Subscribe to our channels for the next episode of Ask The Placenta Lady, or send us your question!![]()
![]()

* Updates to original transcript:
I originally stated the WHO suggests a 5% Cesarean rate world-wide; it’s more like 10%.